Successful Liver transplant from mother to 3 year old child

Amidst #COVID 19, Successful Liver transplant from mother to 3 year old child. The child was suffering from Progressive Familial Intrahepatic Cholestasis #PFIC-3.

Amidst #COVID 19, Successful Liver transplant from mother to 3 year old child. The child was suffering from Progressive Familial Intrahepatic Cholestasis #PFIC-3.

As a doctor, you’ve gone above and beyond everything, I ever would have expected. The world would be a much better place if all of the doctors were like you. No words are enough to appreciate the service you do. Thank you so much for everything that you have done. Love from Bangladesh.


Successful Living Donor Living Transplantation from mother to 4 year child suffering from Progressive Familial Intrahepatic Cholestasis (PFIC -3), amidst #COVID 19.
This video demonstrates our technique of Donor Hepatectomy Surgery using midline incision.
Steps

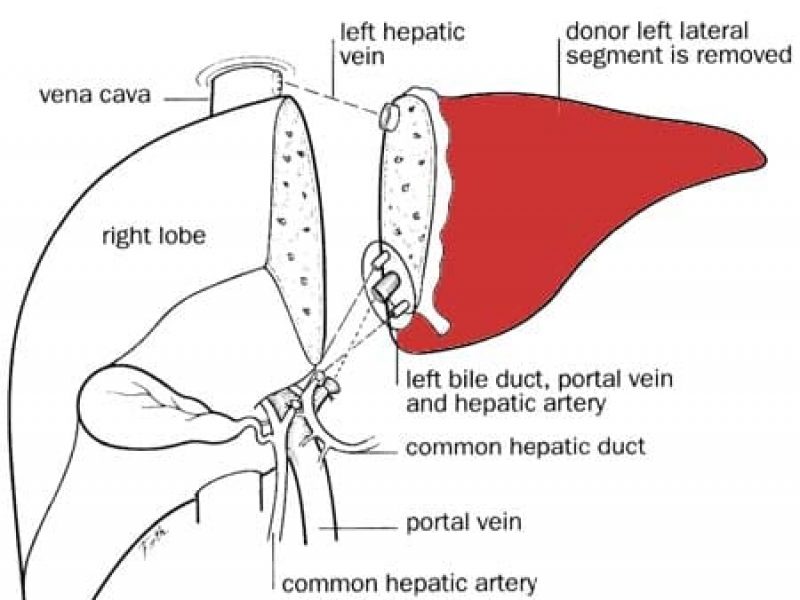
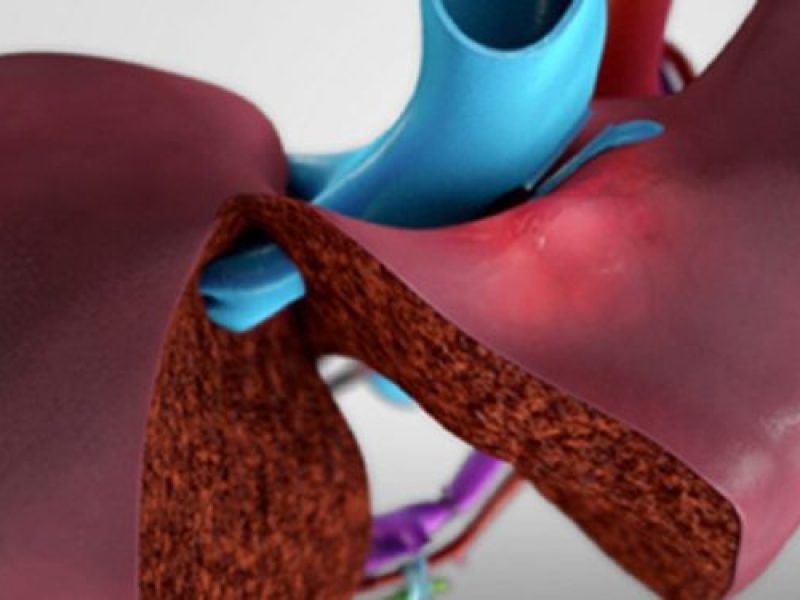
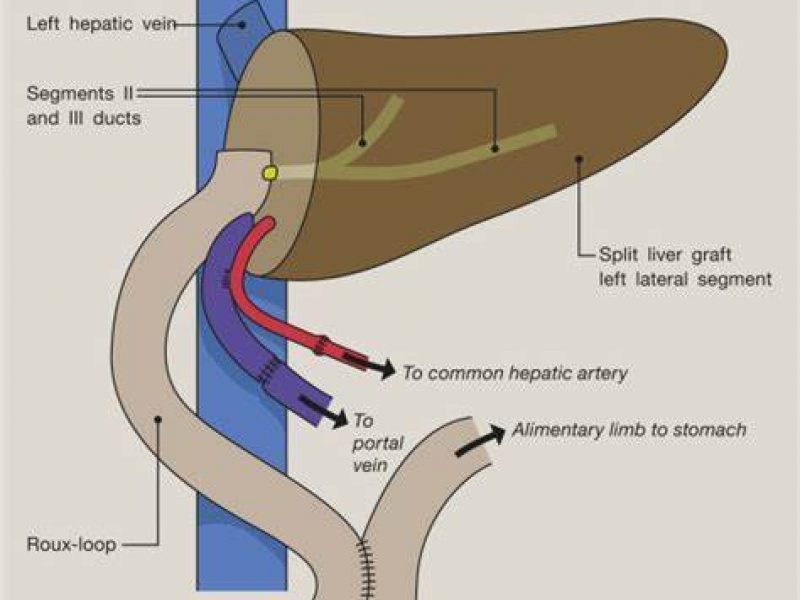
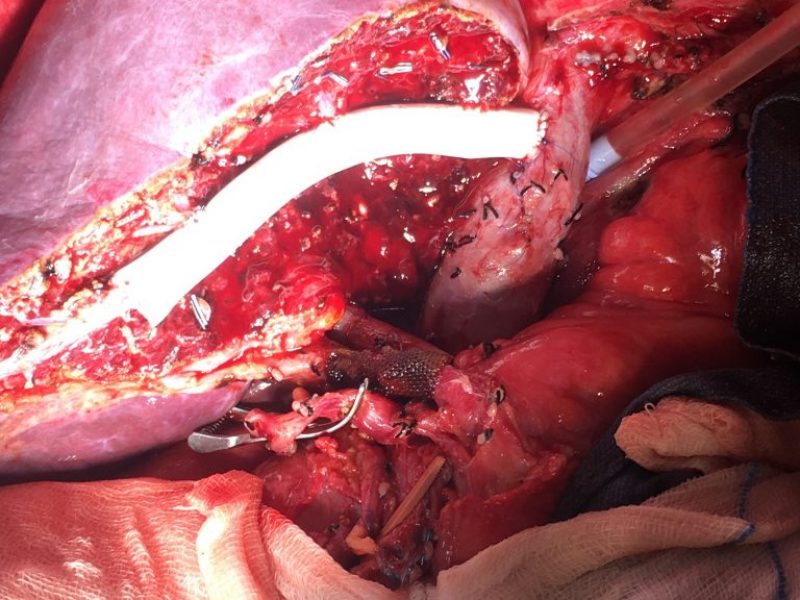
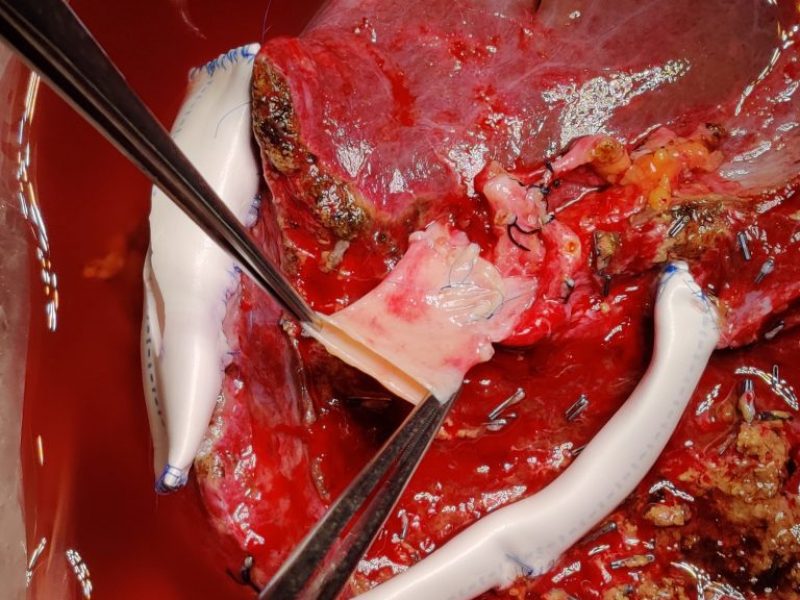
Background: In right lobe adult to adult living donor liver transplantation, ensuring adequate venous outflow is of essence to prevent graft congestion (especially anterior sector congestion), and ensure good graft function in the recipient . The outflow vessels in the right lobe graft include the right hepatic veins (RHV), short hepatic veins (also called right inferior hepatic veins, RIHV’s), and the middle hepatic vein (MHV) tributaries (namely segment 5 and 8 veins). Choice of the type of right graft (with subtotal MHV, partial MHV, or modified rt lobe) depends on remnant volume, metabolic demand of recipient and donor venous anatomy of right lobe; the number of veins that need to be reconstructed accordingly vary.
Aim: In this video, we demonstrate the surgical technique to reconstruct multiple RIHV’s (usually >3mm in size), and multiple MHV tributaries (usually >5 mm, but sometimes 3-5 mm) using synthetic polytetrafluoroethylene (PTFE) grafts in complex right lobe grafts. This reconstruction on the bench, simplifies and expedites anastomoses in the recipient during implantation, thus reducing the warm ischemia time (WIT).
Video description: It is important to ensure a good flush of all the areas of the harvested graft, drained by the small inferior veins and MHV tributaries, some times requiring a “reverse flush” through them in addition to the “forward flush” through the portal vein. Different types of reconstruction techniques in cases with differing right lobe donor anatomy are shown. The first donor, had 2 RIHV’s in different planes which were implanted on to a “boat” PTFE graft of 14 mm on the bench. A neo-MHV was created using a straight 8 mm PTFE extension graft from the donor MHV (subtotal MHV graft). These were then subsequently implanted onto the inferior vena cava (IVC) of the recipient. In the second donor, a right lobe with modified MHV (separate segment 5 and 8 veins) was harvested, and on the bench, the segment 5 and 8 veins were implanted end-to-side and end-to-end on to a PTFE graft, respectively, to create a neo-MHV. The graft function was satisfactory in both cases.
Conclusion: Bench reconstruction of small MHV tributaries and multiple small RIHV’s using synthetic grafts, helps in reducing warm ischemia time, avoids congestion of the partial graft, thereby ensuring good graft function in the recipient.